Análisis de costo-utilidad en Colombia del tratamiento integral del carcinoma de seno con reconstrucción inmediata frente a la reconstrucción diferida
Resumen
Introducción. La reconstrucción mamaria inmediata o diferida hace parte del tratamiento del cáncer de mama. Cada país y sistema de salud costea y evalúa estos procedimientos de forma diferente. Es importante determinar cuál estrategia resulta de mayor costo-utilidad en Colombia.
Objetivo. Evaluar la costo-utilidad del tratamiento del cáncer de mama con reconstrucción inmediata, comparada con la reconstrucción diferida.
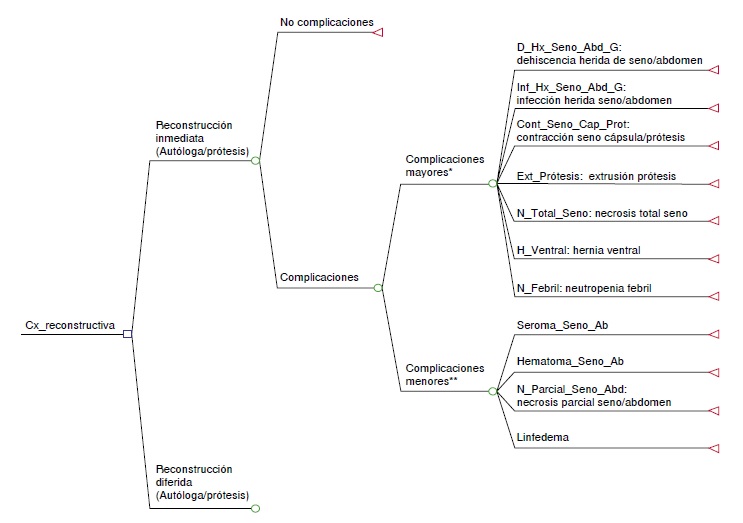
Materiales y métodos. Se utilizó un modelo de árbol de decisiones con un plazo previsto de un año desde la perspectiva del tercer pagador. Los datos de costos se tomaron del manual tarifario del Instituto de Seguros Sociales de 2001 más un ajuste del 30 % según la metodología del Instituto de Evaluación Tecnológica en Salud y el modelo de facturación del Centro Javeriano de Oncología del Hospital Universitario San Ignacio. Las probabilidades de transición y las utilidades se obtuvieron de
médicos especialistas, de las pacientes y de la literatura médica. Se hicieron los análisis univariado y probabilístico de sensibilidad.
Resultados. Los costos esperados per cápita fueron de COP$ 26’710.605 (USD$ 11.165) para la reconstrucción inmediata y de COP$ 6’459.557 (USD$ 11.060) para la diferida. La reconstrucción inmediata generó un costo incremental de COP$ 251.049 (USD$ 105), así como 0,75 años de vida ajustados por calidad (AVAC), en tanto que la diferida generó 0,63 AVAC, con una relación de costoutilidad incremental de COP $2’154.675 por AVAC (USD$ 901).
Conclusiones. El costo por AVAC no superó el umbral de aceptabilidad del producto interno bruto (PIB) per cápita. Los costos durante el primer año resultaron similares y ambas técnicas son favorables para el sistema de salud colombiano, pero la utilidad de la reconstrucción inmediata reportada por los pacientes y en la literatura médica, es mayor.
Descargas
Referencias bibliográficas
International Agency for Research on Cancer. Cancer fact sheets. Fecha de consulta: 1 de junio de 2014. Disponible en: http://gco.iarc.fr/today/fact-sheets-cancers?cancer=15&type=0&sex=2
Instituto Nacional de Cancerología. Incidencia estimada y mortalidad por cáncer en Colombia 2002-2006. p. 39. Fecha de consulta: 1 de junio de 2014. Disponible en: http://www.cancer.gov.co//files/libros/archivos/a9412b1cdffddfb228e09f7d31e9e124_Incidencia%20Estimada%20Y%20Mortalidad%202002-2006.pdf
Colwell AS, Tessler O, Lin AM, Liao E, Winograd J, Cetrulo CL, et al. Breast reconstruction following nipplesparing mastectomy. Plast Reconstr Surg. 2014;133:496-506. https://doi.org/10.1097/01.prs.0000438056.67375.75
Grover R, Padula WV, van Vliet M, Ridgway EB. Comparing five alternative methods of breast reconstruction surgery. Plast Reconstr Surg. 2013;132:709e-23. https://doi.org/10.1097/PRS.0b013e3182a48b10
Giachero-Castaño V, Jacobo-Bastreri O, Grattarola-Rizzo G, Carriquiry-Kayel C. Reconstrucción mamaria con colgajo músculo-cutáneo transverso de recto abdominal [TRAM] y simetrización simultánea. Cir Plast Iberolatinoam. 2010;36:135-44.
Neyt MJ, Blondeel PN, Morrison CM, Albrecht JA. Comparing the cost of delayed and immediate autologous breast reconstruction in Belgium. Br J Plast Surg. 2005;58:493-7. https://doi.org/10.1016/j.bjps.2004.12.002
Thomas RJ, Williams M, Marshall C, Glen J, Callam M. The total hospital and community UK costs of managing patients with relapsed breast cancer. Br J Cancer. 2009;100:598-600. https://doi.org/10.1038/sj.bjc.6604911
Knaul FM, Arreola-Ornelas H, Velázquez E, Dorantes J, Méndez Ó, Ávila-Burgos L. El costo de la atención médica del cáncer mamario: el caso del Instituto Mexicano del Seguro Social. Salud Pública Mex. 2009;51(Supl.2):s286-95.
Palit TK, Miltenburg DM, Brunicardi FC. Cost analysis of breast conservation surgery compared with modified radical mastectomy with and without reconstruction. Am J Surg. 2000;179:441-5. https://doi.org/10.1016/S0002-9610(00)00383-4
Alderman AK, Storey AF, Nair NS, Chung KC. Financial impact of breast reconstruction in academic practice. Plast Reconstr Surg. 2010;123:1408-13. https://doi.org/10.1097/PRS.0b013e3181a0722d
Campbell JD, Ramsey SD. The costs of treating breast cancer in the US. Pharmacoeconomics. 2009;27:199-209. https://doi.org/10.2165/00019053-200927030-00003
Kaliks RA, Pontes LD, Bognar CL, Santos KC, Bromberg SE, do Amaral PG, et al. Treatment of breast cancer patients from a public healthcare system in a private center: Costs of care for a pilot public-private partnership in oncology. Einstein (Sao Paulo). 2013;11:216-23. https://doi.org/10.1590/S1679-45082013000200014
Atherton DD, Hills AJ, Moradi P, Muirhead N, Wood SH. The economic viability of breast reconstruction in the UK: Comparison of a single surgeon’s experience of implant; LD; TRAM and DIEP based reconstructions in 274 patients. J Plast Reconstr Aesthet Surg. 2011;64:710-5. https://doi.org/10.1016/j.bjps.2010.11.001
Albornoz CR, Cordeiro PG, Mehrara BJ, Pusic AL, McCarthy CM, Disa JJ, et al. Economic implications of recent trends in U.S. immediate autologous breast reconstruction. Plast Reconstr Surg. 2014;133:463-70. https://doi.org/10.1097/PRS.0000000000000039
Israeli R, Funk S, Reaven NL. Comparative analysis of 18-month outcomes and costs of breast reconstruction flap procedures. Plast Reconstr Surg. 2014;133:471-9. https://doi.org/10.1097/PRS.0000000000000064
Paget JT, Young KC, Wilson SM. Accurately costing unilateral delayed DIEP flap breast reconstruction. J Plast Reconstr Aesthetic Surg. 2013;66:926-30. https://doi.org/10.1016/j.bjps.2013.03.032
Thoma A, Veltri K, Khuthaila D, Rockwell G, Duku E. Comparison of the deep inferior epigastric perforator flap and free transverse rectus abdominis myocutaneous flap in postmastectomy reconstruction: A cost-effectiveness analysis. Plast Reconstr Surg. 2004;113:1650-61. https://doi.org/10.1097/01.PRS.0000117196.61020.FD
Thoma A, Khuthaila D, Rockwell G, Veltri K. Cost-utility analysis comparing free and pedicled TRAM flap for breast reconstruction. Microsurgery. 2003;23:287-95. https://doi.org/10.1002/micr.10138
Spear SL, Mardini S, Ganz JC. Resource cost comparison of implant-based breast reconstruction versus TRAM flap breast reconstruction. Plast Reconstr Surg. 2003;112:101-5. https://doi.org/10.1097/01.PRS.0000066007.06371.47
Rosenqvist S, Sandelin K, Wickman M. Patients’ psychological and cosmetic experience after immediate breast reconstruction. Eur J Surg Oncol. 1996;22:262-6.
Rowland JH, Katherine A, Meyerowitz BE, Belin TR, Wyatt GE, Ganz PA. Role of breast reconstructive surgery in physical and emotional outcomes among breast cancer survivors. J Natl Cancer Inst. 2000;92:1422-9. Erratum in: J Natl Cancer Inst. 2001;93:68.
Mullan MH, Wilkins EG, Goldfarb S, Lowery JC, Smith DM, Wickman M, et al. Prospective analysis of psychosocial outcomes after breast reconstruction: Crosscultural comparisons of 1-year postoperative results. J Plast Reconstr Aesthet Surg. 2007;60:503-8. https://doi.org/10.1016/j.bjps.2005.10.033
Atisha D, Alderman AK, Lowery JC, Kuhn LE, Davis J, Wilkins EG. Prospective analysis of long-term psychosocial outcomes in breast reconstruction: Two-year postoperative results from the Michigan Breast Reconstruction Outcomes Study. Ann Surg. 2008;247:1019-28. https://doi.org/10.1097/SLA.0b013e3181728a5c
Schain WS, Wellisch DK, Pasnau RO, Landsverk J. The sooner the better: A study of pshycological factors in women undergoing immediate versus delayed breast reconstruction. Am J Psychiatry. 1985;142:40-6. https://doi.org/10.1176/ajp.142.9.A40
Guyomard V, Leinster S, Wilkinson M. Systematic review of studies of patients’ satisfaction with breast reconstruction after mastectomy. Breast. 2007;16:547-67. https://doi.org/10.1016/j.breast.2007.04.004
Soares PB, Carneiro JA, Rocha LA, Gonçalves RC, Martelli DR, Silveira MF, et al. The quality of life of disease-free Brazilian breast cancer survivors. Rev Esc Enferm USP. 2013;47:69-75. https://doi.org/10.1590/S0080-62342013000100009
Elder EE, Brandberg Y, Björklund T, Rylander R, Lagergren J, Jurell G, et al. Quality of life and patient satisfaction in breast cancer patients after immediate breast reconstruction: A prospective study. Breast. 2005;14:201-8. https://doi.org/10.1016/j.breast.2004.10.008
Rute de Oliveira R, Morais SS, Sarian LO. Efeitos da reconstrução mamária imediata sobre a qualidade de vida de mulheres mastectomizadas. Rev Bras Ginecol Obs. 2010;32:602-8. https://doi.org/10.1590/S0100-72032010001200007
Al-Ghazal SK, Sully L, Fallowfield L, Blamey RW. The psychological impact of immediate rather than delayed breast reconstruction. Eur J Surg Oncol. 2000;26:17-9.
https://doi.org/10.1053/ejso.1999.0733
Al-Ghazal SK, Fallowfield L, Blamey RW. Comparison of psychological aspects and patient satisfaction following breast conserving surgery, simple mastectomy and breast reconstruction. Eur J Cancer. 2000;36:1938-43. https://doi.org/10.1016/S0959-8049(00)00197-0
Cocquyt VF, Blondeel PN, Depypere HT, van De Sijpe KA, Daems KK, Monstrey SJ, et al. Better cosmetic results and comparable quality of life after skin-sparing mastectomy and immediate autologous breast reconstruction compared to breast conservative treatment. Br J Plast Surg. 2003;56:462-70. https://doi.org/10.1016/S0007-1226(03)00198-X
Sullivan PW, Green V. Preference-based EQ-5D index scores for chronic conditions in the United States. Med Decis Mak. 2006;26:410-20. https://doi.org/10.1177/0272989X06290495
Alderman AK, Kuhn LE, Lowery JC, Wilkins EG. Does patient satisfaction with breast reconstruction change over time? Two-year results of the Michigan Breast Reconstruction Outcomes Study. J Am Coll Surg. 2007;204:7-12. https://doi.org/10.1016/j.jamcollsurg.2006.09.022
Contant CM, van Wersch AM, Wiggers T, Wai RT, van Geel AN. Motivations, satisfaction, and information of immediate breast reconstruction following mastectomy. Patient Educ Couns. 2000;40:201-8. https://doi.org/10.1016/S0738-3991(99)00078-6
Veiga DF, Sabino Neto M, Ferreira LM, García EB, Veiga Filho J, Novo NF, et al. Quality of life outcomes after pedicled TRAM flap delayed breast reconstruction. Br J Plast Surg. 2004;57:252-7. https://doi.org/10.1016/j.bjps.2003.12.029
Lee C, Sunu C, Pignone M. Patient-reported outcomes of breast reconstruction after mastectomy: A systematic review. J Am Coll Surg. 2009;209:123-33. https://doi.org/10.1016/j.jamcollsurg.2009.02.061
Pusic AL, Klassen AF, Scott AM, Klok JA, Cordeiro PG, Cano SJ. Development of a new patient-reported outcome measure for breast surgery: The BREAST-Q. Plast Reconstr Surg. 2009;124:345-53. https://doi.org/10.1097/PRS.0b013e3181aee807
Drummond MF, Sculpher MJ, Torrace GW, O’Brien BJ. Methods for the economic evaluation of health care programmes. Third edition. Oxford: Oxford University Press; 2005.
Preminger BA, Pusic AL, McCarthy CM, Verma N, Worku A, Cordeiro PG. How should quality-of-life data be incorporated into a cost analysis of breast reconstruction? A consideration of implant versus free TRAM flap procedures. Plast Reconstr Surg. 2008;121:1075-82. https://doi.org/10.1097/01.prs.0000304246.66477.cd
Instituto de Evaluación Tecnológica en Salud. Manual para la elaboración de evaluaciones económicas en salud. Bogotá D.C.: IETS; 2014.
Cochrane Training. Manual Cochrane de revisiones sistemáticas de intervenciones. Version 5. Londres: The Cochrane Collaboration; 2011.
Tufts Medical Center, Institute for Clinical Research and Health Policy. Cost-effectiveness analysis registry/Searching de CEA registry/Search the CEA Registry / Basic search/Utility Weights / Full Search Contents: Breast reconstruction. Fecha de consulta: 1 de agosto de 2013. Disponible en: http://healtheconomics.tuftsmedicalcenter.org/cear4/SearchingtheCEARegistry/SearchtheCEARegistry.aspx
Centre for Evidence-Based Medicine. Resources: Levels of evidence. Fecha de consulta: 2 de abril de 2014. Disponible en: https://www.cebm.net/2009/06/oxford-centreevidence-based-medicine-levels-evidence-march-2009/
GRADE Working Group. What is “quality of evidence” and why is it important to clinicians? BMJ. 2008;336:995. https://doi.org/10.1136/bmj.39490.551019.BE
Husereau D, Drummond M, Petrou S, Carswell C, Moher D, Greenberg D, et al. Consolidated Health Economic Evaluation Reporting Standards (CHEERS) statement. Eur J Heal Econ. 2013;14:367-72.
Lu SM, Nelson JA, Fischer JP, Fosnot J, Goldstein J, Selber JC, et al. The impact of complications on function, health, and satisfaction following abdominally based autologous breast reconstruction: A prospective evaluation. J Plast Reconstr Aesthet Surg. 2014;67:682-92. https://doi.org/10.1016/j.bjps.2014.01.017
Carnevale A, Scaringi C, Scalabrino G, Campanella B, Osti MF, De Sanctis V, et al. Radiation therapy after breast reconstruction: Outcomes, complications, and patient satisfaction. Radiol Med. 2013;118:1240-50. https://doi.org/10.1007/s11547-013-0947-6
Sullivan SR, Fletcher DRD, Isom CD, Isik FF. True incidence of all complications following immediate and delayed breast reconstruction. Plast Reconstr Surg. 2008;122:19-28. https://doi.org/10.1097/PRS.0b013e3181774267
Jiménez-Puente A, Prieto-Lara E, Rueda-Domínguez A, Maañón-Di Leo C, Benítez-Parejo N, Rivas-Ruiz F, et al. Complications in immediate breast reconstruction after mastectomy. Int J Technol Assess Health Care. 2011;27:298-304. https://doi.org/10.1017/S026646231100047X
Tribondeau P, Soffray F. Reconstruction mammaire par lambeau musculocutané unipédiculé de muscle grand droit de l’abdomen (115 cas consécutifs). Ann Chir Plast Esthet. 2008;53:309-17. https://doi.org/10.1016/j.anplas.2007.05.009
Weycker D, Edelsberg J, Kartashov A, Barron R, Lyman G. Risk and healthcare costs of chemotherapy-induced neutropenic complications in women with metastatic breast cancer. Chemotherapy. 2012;58:8-18. https://doi.org/10.1159/000335604
Chie WC, Huang CS, Chen JH, Chang K. Utility assessment for different clinical phases of breast cancer in Taiwan. J Formos Med Assoc. 2000;99:677-83.
Chang DW, Kim S. Breast reconstruction and lymphedema. Plast Reconstr Surg. 2010;125:19-23. https://doi.org/10.1097/PRS.0b013e3181c49477
Instituto de Seguros Sociales. Acuerdo No. 256 de 2001. Fecha de consulta: 2 de junio de 2014. Disponible en: http://www.hrd.gov.co/documentos/facturacion/MANUAL%20DE%20FACTURACION%202013/TARIFAS%20ISS%20-01%20AC256.pdf.
Sistema Integral de Información de la Protección Social. Regulación de precios. Termómetro de precios de medicamentos. Publicación precios reportados 201401a201403
(fecha de creación 2014-06-27). Fecha de consulta: 3 de septiembre de 2014. Disponible en: http://web.sispro.gov.co/WebPublico/Consultas/ConsultarCNPMCadenaComercializacionCircu2yPA_028_2_2.aspx.
Thompson SG, Nixon RM. How sensitive are costeffectiveness analyses to choice of parametric distributions? Med Decis Making. 2015;25:416-23. https://doi.org/10.1177/0272989X05276862
Skedgel C, Rayson D, Younis T. Is adjuvant trastuzumab a cost-effective therapy for HER-2/neu-positive T1bN0 breast cancer? Ann Oncol. 2013;24:1834-40. https://doi.org/10.1093/annonc/mdt069
Cheville AL, Almoza M, Courmier JN, Basford JR. A prospective cohort study defining utilities using time tradeoffs and the Euroqol-5D to assess the impact of cancerrelated lymphedema. Cancer. 2010;116:3722-31. https://doi.org/10.1002/cncr.25068
Ko CY, Maggard M, Livingston EH. Evaluating health utility in patients with melanoma, breast cancer, colon cancer, and lung cancer: A nationwide, population-based assessment. J Surg Res. 2003;114:1-5. https://doi.org/10.1016/S0022-4804(03)00167-7
TreeAge Software, Inc. Software I. Williamstown: TreeAge Software, Inc.; 2014.
Urrutia G, Bonfill X. Declaración PRISMA: una propuesta para mejorar la publicación de revisiones sistemáticas y metaanálisis. Med Clin (Barc). 2010;135:507-11. https://doi.org/10.1016/j.medcli.2010.01.015
Albornoz CR, Cordeiro PG, Pusic AL, McCarthy CM, Mehrara BJ, Disa JJ, et al. Diminishing relative contraindications for immediate breast reconstruction: A multicenter study. J Am Coll Surg. 2014;219:788-95. https://doi.org/10.1016/j.jamcollsurg.2014.05.012
Veronesi U, Cascinelli N, Mariani L, Greco M, Saccozzi R, Luini A, et al. Twenty-year follow-up of a randomized study comparing breast-conserving surgery with radical mastectomy for early breast cancer. N Engl J Med. 2002;347:1227-32. https://doi.org/10.1056/NEJMoa020989
Monrigal E, Dauplat J, Gimbergues P, Le Bouedec G, Peyronie M, Achard JL, et al. Mastectomy with immediate breast reconstruction after neoadjuvant chemotherapy and radiation therapy. A new option for patients with operable invasive breast cancer. Results of a 20 years single institution study. Eur J Surg Oncol. 2011;37:864-70. https://doi.org/10.1016/j.ejso.2011.07.009
Nedumpara T, Jonker L, Williams MR. Impact of immediate breast reconstruction on breast cancer recurrence and survival. Breast. 2011;20:437-43. https://doi.org/10.1016/j.breast.2011.04.006
Tsoi B, Ziolkowski NI, Thoma A, Campbell K, O’Reilly D, Goeree R. Systematic review on the patient-reported outcomes of tissue-expander/ implant vs autologous abdominal tissue breast reconstruction in postmastectomy breast cancer patients. J Am Coll Surg. 2014;218:1038-48. https://doi.org/10.1016/j.jamcollsurg.2014.02.011
Thoma A, Jansen L, Sprague S, Stat ED. A comparison of the superficial inferior epigastric artery flap and deep inferior epigastric perforator flap in postmastectomy reconstruction: A cost-effectiveness analysis incremental effectiveness. Can J Plast Surg. 2008;16:77-84.
Munhoz AM, Aldrighi CM, Montag E, Arruda EG, Aldrighi JM, Gemperli R, et al. Clinical outcomes following nippleareola-sparing mastectomy with immediate implant-based breast reconstruction: A 12-year experience with an analysis of patient and breast-related factors for complications. Breast Cancer Res Treat. 2013;140: 545-55. https://doi.org/10.1007/s10549-013-2634-7
Ruiz M, Rejas J, Soto J, Pardo A, Rebollo I. Adaptación y validación del Health Utilities Index Mark 3 al castellano y baremos de corrección en la población española. Med Clin (Barc). 2003;120:89-96.
Horsman J, Furlong W, Feeny D, Torrance G. The Health Utilities Index (HUI): concepts, measurement properties and applications. Health Qual Life Outcomes. 2003;1:54. https://doi.org/10.1186/1477-7525-1-54
Zarate V, Kind P, Valenzuela P, Vignau A, Olivares-Tirado P, Muñoz A. Social valuation of EQ-5D health states: The Chilean case. Value Health. 2011;14:1135-41. https://doi.org/10.1016/j.jval.2011.09.002
Herdman M, Badia X, Berra S. El EuroQol-5D: una alternativa sencilla para la medición de la calidad de vida relacionada con la salud en atención primaria. Atención Primaria. 2001;28:425-9.
Pickard AS, De Leon MC, Kohlmann T, Cella D, Rosenbloom S. Psychometric comparison of the standard EQ-5D to a 5 level version in cancer patients. Med Care. 2007;45: 259-63. https://doi.org/10.1097/01.mlr.0000254515.63841.81
Parker P, Youssef A, Walker S, Basen-Engquist K, Cohen L, Gritz ER, et al. Short-term and long-term psychosocial adjustment and quality of life in women undergoing different surgical procedures for breast cancer. Ann Surg Oncol. 2007;14:3078-89.
Herdman M, Gudex C, Lloyd A, Janssen M, Kind P, Parkin D, et al. Development and preliminary testing of the new five-level version of EQ-5D (EQ-5D-5L). Qual Life Res. 2011;20:1727-36. https://doi.org/10.1007/s11136-011-9903-x
Dolan P, Gudex C, Kind P, Williams A. Valuing health states: A comparison of methods. J Health Econ. 1996;15: 209-31. https://doi.org/10.1016/0167-6296(95)00038-0
Brady MJ, Cella DF, Mo F, Bonomi AE, Tulsky DS, Lloyd SR, et al. Reliability and validity of the functional assessment of cancer therapy-breast quality-of-life instrument. J Clin Oncol. 1997;15:974-86.
Pradas-Velasco R, Villar FA, Puy-Martínez-Zárate M. Utilización del cuestionario European Quality of Life-5 Dimensions (EQ-5D) para valorar la variación de la calidad de vida relacionada con la salud debida a la gripe. Gac Sanit. 2009;23:104-8.
Cheng MH, Lin JY, Ulusal BG, Wei FC. Comparisons of resource costs and success rates between immediate and delayed breast reconstruction using DIEP or SIEA flaps under a well-controlled clinical trial. Plast Reconstr Surg. 2006;117:2139-42. https://doi.org/10.1097/01.prs.0000218286.64522.15
von Minckwitz G, Schwenkglenks M, Skacel T, Lyman GH, Pousa AL, Bacon P, et al. Febrile neutropenia and related complications in breast cancer patients receiving pegfilgrastim primary prophylaxis versus current practice neutropaenia management: Results from an integrated analysis. Eur J Cancer. 2009;45:608-17. https://doi.org/10.1016/j.ejca.2008.11.021
Bennett CL, Calhoun EA. Evaluating the total costs of chemotherapy-induced febrile neutropenia: Results from a pilot study with community oncology cancer patients. Oncologist. 2007;12:478-83. https://doi.org/10.1634/theoncologist.12-4-478
Chan A, Chen C, Chiang J, Tan SH, Ng R. Incidence of febrile neutropenia among early-stage breast cancer patients receiving anthracycline-based chemotherapy. Support Care Cancer. 2012;20:1525-32. https://doi.org/10.1007/s00520-011-1241-6
Gandhi SK, Arguelles L, Boyer JG. Economic impact of neutropenia and febrile neutropenia in breast cancer: Estimates from two national databases. Pharmacotherapy.
;21:684-90. https://doi.org/10.1592/phco.21.7.684.34568
Algunos artículos similares:
- Constanza Pardo, Ricardo Cendales, Supervivencia de pacientes con cáncer de cuello uterino tratadas en el Instituto Nacional de Cancerología , Biomédica: Vol. 29 Núm. 3 (2009)
- Concepción Judith Puerta, Paula Ximena Pavia, Marleny Montilla, Carolina Flórez, Giomar Herrera, Juan Manuel Ospina, Fred Manrique, Rubén Santiago Nicholls, Reporte del primer caso de enfermedad de Chagas transplacentaria analizado por AP-PCR en Moniquirá, Boyacá , Biomédica: Vol. 29 Núm. 4 (2009)
- Yolanda Lucía López, Claudia González, Berta Natalia Gallego, Ana Lida Moreno, Rectoría de la vigilancia en salud pública en el sistema de seguridad social en salud de Colombia: estudio de casos , Biomédica: Vol. 29 Núm. 4 (2009)
- Oscar Fernando Herrán, María F. Ardila, Tipología de los consumidores de alcohol y sus factores determinantes en Bucaramanga, Colombia , Biomédica: Vol. 29 Núm. 4 (2009)
- Óscar Gamboa, Sandra Díaz, Liliana Chicaíza, Mario García, Análisis de costo-efectividad en Colombia de anastrazol Vs. tamoxifeno como terapia inicial en mujeres con cáncer temprano de mama y receptor hormonal positivo , Biomédica: Vol. 30 Núm. 1 (2010)
- María del Pilar Chaves, Julián Alfredo Fernández, Isabel Ospina, Myriam Consuelo López, Ligia Moncada, Patricia Reyes, Tendencia de la prevalencia y factores asociados a la infección por Giardia duodenalis en escolares y preescolares de una zona rural de Cundinamarca , Biomédica: Vol. 27 Núm. 3 (2007)
- Dolly Marcela Zapata, Alejandro Estrada, Calidad de vida relacionada con la salud de las personas afectadas por quemaduras después de la cicatrización, Medellín, Colombia , Biomédica: Vol. 30 Núm. 4 (2010)
- Wilson Mejía, Carlos Castro, Adriana Umaña, Clemencia de Castro, Tulia Riveros, Myriam Sánchez-Gómez, Señalización asociada al receptor del factor de crecimiento similar a la insulina de tipo I en una línea celular colombiana de carcinoma mamario , Biomédica: Vol. 30 Núm. 4 (2010)
- Alejandro Estrada, Doris Cardona, Ángela María Segura, Lina Marcela Chavarriaga, Jaime Ordóñez, Jorge Julián Osorio, Calidad de vida de los adultos mayores de Medellín , Biomédica: Vol. 31 Núm. 4 (2011)
- Jaiberth Cardona-Arias, Luz Peláez-Vanegas, Juan López-Saldarriaga, Marcela Duque-Molina, Oscar Leal-Álvarez, Calidad de vida relacionada con la salud en adultos con VIH/sida, Medellín, Colombia, 2009 , Biomédica: Vol. 31 Núm. 4 (2011)
| Estadísticas de artículo | |
|---|---|
| Vistas de resúmenes | |
| Vistas de PDF | |
| Descargas de PDF | |
| Vistas de HTML | |
| Otras vistas | |

























