Efectos del ejercicio físico sobre la cognición en mujeres mayores tratadas con lovastatina
Resumen
Introducción. El deterioro cognitivo tiene una gran incidencia en el adulto mayor.
Objetivo. El principal objetivo de este estudio fue analizar los efectos sobre la cognición y la concentración de lípidos de un programa de caminatas en mujeres mayores de 60 años tratadas con lovastatina.
Materiales y métodos. Las participantes se distribuyeron en dos grupos: uno con ejercicio (EG, n=45) sometido a entrenamiento aeróbico y otro inactivo o sedentario (SG, n=22). El estado cognitivo se evaluó mediante la versión en español del Mini-Mental Test. Los niveles de lipoproteínas se midieron con una prueba de perfil lipídico y la aptitud cardiorrespiratoria se valoró con la prueba de caminata de 6 minutos (Six-Minute Walking Test, 6MWT).
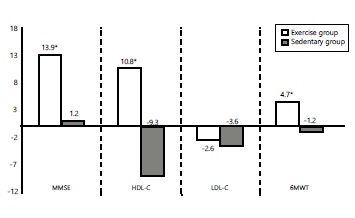
Resultados. El grupo con ejercicio mostró una mejora significativa (p<0,05) de la aptitud cardiorrespiratoria y de las concentraciones de colesterol HDL. Además, en la prueba de cognición se observó un efecto de gran tamaño en la orientación espacial, en la atención y en el cálculo. La reducción del colesterol LDL no fue significativa.
Conclusión. Un programa de entrenamiento progresivo y supervisado para mujeres mayores tratadas con lovastatina, podría mejorar la actividad cerebral relacionada con el colesterol HDL, lo cual podría retrasar el deterioro cognitivo.
Descargas
Referencias bibliográficas
Allison MA, Jensky NE, Marshall SJ, Bertoni AG, Cushman M. Sedentary behavior and adiposity-associated inflammation: The multi-ethnic study of atherosclerosis. Am J Prev Med. 2012;42:8-13. https://doi.org/10.1016/j.amepre.2011.09.023
Koh Y, Ben-Ezra V, Biggerstaff KD, Nichols DL. Responses of blood lipids and lipoproteins to extendedrelease niacin and exercise in sedentary postmenopausal women. J Gerontol A Biol Sci Med Sci. 2010;65:924-32. https://doi.org/10.1093/gerona/glq097
Jong-Hwan P, Masashi M, Masaki T, Noriaki K, Harumi H, Hyun-Shik K, et al. Low-volume walking program improves cardiovascular-related health in older adults. J Sports Sci Med. 2014;13:624-31.
van den Kommer TN, Dik MG, Comijs HC, Jonker C, Deeg DJH. The role of lipoproteins and inflammation in cognitive decline: Do they interact? Neurobiol Aging. 2012;33:196.e1-96.e12. https://doi.org/10.1016/j.neurobiolaging.2010.05.024
Lucio Mazini Filho M, Gama de Matos D, Minelli Rodrigues B, Jose Aidar F, Rezende de Oliveira Venturini G, da Silva Salgueiro R, et al. The effects of 16 weeks of exercise on metabolic parameters, blood pressure, body mass index and functional autonomy in elderly women. Int Spotmed J. 2013;14:86-93.
Sang-Ho L, Byoung-Do S, Sang-Mi C. The effect of walking exercise on physical fitness and serum lipids in obese middle-aged women: Pilot study. J Phys Ther Sci. 2013;25:1533-6. https://doi.org/10.1589/jpts.25.1533
Kosmidou KV, Douda HT, Eleftheriadou AI, Volaklis KA, Tokmakidis SP. The effect of a 3-year combined exercise program on body composition and lipid profile in elderly women. Archives of Hellenic Medicine. 2014;31:191-9.
Hayashino Y, Jackson JL, Fukumori N, Nakamura F, Fukuhara S. Effects of supervised exercise on lipid profiles and blood pressure control in people with type 2 diabetes mellitus: A meta-analysis of randomized controlled trials. Diabetes Res Clin Pract. 2012;98:349-60. https://doi.org/10.1016/j.diabres.2012.10.004
Greene NP, Martin SE, Crouse SF. Acute exercise and training alter blood lipid and lipoprotein profiles differently in overweight and obese men and women. Obesity. 2012;20:1618-27. https://doi.org/10.1038/oby.2012.65
Macoris Colombo C, Michel de Macedo R, Morita Fernandes-Silva M, Moro Caporal A, Emilia Stinghen A, Roberto Costantini C, et al. Short-term effects of moderate intensity physical activity in patients with metabolic syndrome. Einstein (Sao Paulo). 2013;11:324-30. http://doi. org/10.1590/S1679-45082013000300011
Lippi G, Schena F, Salvagno GL, Montagnana M, Ballestrieri F, Guidi GC. Comparison of the lipid profile and lipoprotein(a) between sedentary and highly trained subjects. Clin Chem Lab Med. 2006;44:322-6. https://doi.org/10.1515/CCLM.2006.056
Kodama S, Tanaka S, Saito K, Shu M, Sone Y, Onitake F, et al. Effect of aerobic exercise training on serum levels of high-density lipoprotein cholesterol: A meta-analysis. Arch Intern Med. 2007;167:999-1008. https://doi.org/10.1001/archinte.167.10.999
Wooten JS, Biggerstaff KD, Ben-Ezra V. A single 1-h session of moderate-intensity aerobic exercise does not modify lipids and lipoproteins in normolipidemic obese women. Appl Physiol Nutr Metab. 2011;36:715-22. https://doi.org/110.1139/h11-090
Boardley D, Fahlman M, Topp R, Morgan AL, McNevin N. The impact of exercise training on blood lipids in older adults. Am J Geriatr Cardiol. 2007;16:30-5.
Čaparevič Z, Kostič N, Čelič V, Čosič Z, Marina D, Ilič S, et al. Effects of acute exercise on atherogenic lipids in untreated mild hypertensive patients. Vojnosanit Pregl. 2009;66:313-8.
Tjønna AE, Lee SJ, Rognmo Ø, Stølen TO, Bye A, Haram PM, et al. Aerobic interval training versus continuous moderate exercise as a treatment for the metabolic syndrome: A pilot study. Circulation. 2008;118:346-54. https://doi.org/10.1161/CIRCULATIONAHA.108.772822
Martins RA, Veríssimo MT, Coelho e Silva MJ, Cumming SP, Teixeira AM. Effects of aerobic and strength-based training on metabolic health indicators in older adults. Lipids Health Dis. 2010;9:76. https://doi.org/10.1186/1476-511X-9-76
Bateman LA, Slentz CA, Willis LH, Shields AT, Piner LW, Bales CW, et al. Comparison of aerobic versus resistance exercise training effects on metabolic syndrome (from the Studies of a Targeted Risk Reduction Intervention Through Defined Exercise - STRRIDE-AT/RT). Am J Cardiol. 2011;108:838-44. https://doi.org/10.1016/j.amjcard. 2011.04.037
Poolsup N, Suksomboon N, Wongyaowarat K, Rungkanchananon B, Niyomrat P, Kongsuwan S. Metaanalysis of the comparative efficacy and safety of pitavastatin and atorvastatin in patients with dyslipidaemia. J Clin Pharm Ther. 2012;37:166-72. https://doi.org/10.1111/j.1365-2710.2011.01274.x
Semple SJ. Statin therapy, myopathy and exercise--a case report. Lipids Health Dis. 2012;11:40. https://doi.org/10.1186/1476-511X-11-40
Davignon J. Pleiotropic effects of pitavastatin. Br J Clin Pharmacol. 2012;73:518-35. https://doi.org/10.1111/j.1365-2125.2011.04139.x
Benito-León J, Louis ED, Vega S, Bermejo-Pareja F. Statins and cognitive functioning in the elderly: A populationbased study. J Alzheimers Dis. 2010;21:95-102. https://doi.org/10.3233/JAD-2010-100180
Ghodke R, Tour N, Devi K. Effects of statins and cholesterol on memory functions in mice. Metab Brain Dis. 2012;27:443-51. https://doi.org/10.1007/s11011-012-9343-5
Carlsson CM, Gleason CE, Hess TM, Moreland KA, Blazel HM, Koscik RL, et al. Effects of simvastatin on cerebrospinal fluid biomarkers and cognition in middle-aged adults at risk for Alzheimer’s disease. J Alzheimers Dis. 2008;13:187-97. https://doi.org/10.3233/JAD-2008-13209
Smith KB, Kang P, Sabbagh MN. The effect of statins on rate of cognitive decline in mild cognitive impairment. Alzheimers Dement (N Y). 2017;3:149-56. https://doi.org/10.1016/j.trci.2017.01.001
van Vliet P. Cholesterol and late-life cognitive decline. J Alzheimers Dis. 2012;30(Suppl.2):S147-62. https://doi.org/10.3233/JAD-2011-111028
Bunt CW, Hogan AJ. The effect of statins on dementia and cognitive decline. Am Fam Physician. 2017;95:151-2.
Li R, Wang TJ, Lyu PY, Liu Y, Chen WH, Fan MY, et al. Effects of plasma lipids and statins on cognitive function. Chin Med J. 2018;131:471-6. https://doi.org/10.4103/0366-6999.225062
Reynolds CA, Gatz M, Prince JA, Berg S, Pedersen NL. Serum lipid levels and cognitive change in late life. J Am Geriatr Soc. 2010;58:501-9. https://doi.org/10.1111/j.1532-5415.2010.02739.x
Parnowski T, Kałua B. Global cardio - metabolic risk in pati-ents with cognitive dysfunction. Archives of Psychiatry & Psychotherapy. 2012;14:15-9.
Meusel LA, Anderson ND, Parrott MD, Yuen W, Tchistiakova E, MacIntosh BJ, et al. Brain function is linked to LDL cholesterol in older adults with cardiovascular risk. J Am Geriatr Soc. 2017;65:e51-5. https://doi.org/110.1111/jgs.14663
McGrowder D, Riley C, Morrison EY, Gordon L. The role of high-density lipoproteins in reducing the risk of vascular diseases, neurogenerative disorders, and cancer. Cholesterol. 2011:2011:496925. https://doi.org/10.1155/2011/496925
Packard CJ, Westendorp RG, Stott DJ, Caslake MJ, Murray HM, Shepherd J, et al. Association between apolipoprotein E4 and cognitive decline in elderly adults. J Am Geriatr Soc. 2007;55:1777-85. https://doi.org/10.1111/j.1532-5415.2007.01415.x
Langlois F, Vu TT, Chassé K, Dupuis G, Kergoat M-J,Bherer L. Benefits of physical exercise training on cognition and quality of life in frail older adults. J Gerontol B Psychol Sci Soc Sci. 2013;68:400-4. https://doi.org/10.1093/geronb/gbs069
Yoon JE, Lee SM, Lim HS, Kim TH, Jeon JK, Mun MH. The effects of cognitive activity combined with active extremity exercise on balance, walking activity, memory level and quality of life of an older adult sample with dementia. J Phys Ther Sci. 2013;25:1601-4. https://doi.org/10.1589/jpts.25.1601
Snowden M, Steinman L, Mochan K, Grodstein F, Prohaska TR, Thurman DJ, et al. Effect of exercise on cognitive performance in community‐dwelling older adults: Review of intervention trials and recommendations for public health practice and research. J Am Geriatr Soc. 2011;59:704-16. https://doi.org/10.1111/j.1532-5415.2011.03323.x
Briken S, Gold SM, Patra S, Vettorazzi E, Harbs D, Tallner A, et al. Effects of exercise on fitness and cognition in progressive MS: A randomized, controlled pilot trial. Mult Scler. 2014;20:382-90. https://doi.org/10.1177/1352458513507358
Meeusen R. Exercise, nutrition and the brain. Sports Med. 2014;44(Suppl.1):47-56. https://doi.org/10.1007/s40279-014-0150-5
Andrade LP, Gobbi LT, Coelho FG, Christofoletti G, Riani Costa JL, Stella F. Benefits of multimodal exercise intervention for postural control and frontal cognitive functions in individuals with Alzheimer’s disease: A controlled trial. J Am Geriatr Soc. 2013;61:1919-26. https://doi.org/10.1111/jgs.12531
Mang CS, Campbell KL, Ross CJ, Boyd LA. Promoting neuroplasticity for motor rehabilitation after stroke: Considering the effects of aerobic exercise and genetic variation on brain-derived neurotrophic factor. Phys Ther. 2013;93:1707-16. https://doi.org/10.2522/ptj.20130053
Masley S, Roetzheim R, Gualtieri T. Aerobic exercise enhances cognitive flexibility. J Clin Psychol Med Settings. 2009;16:186-93. https://doi.org/10.1007/s10880-009-9159-6.
Stroth SK. Aerobic endurance exercise benefits memory and affect in young adults. Neuropsychol Rehabil. 2009;19:223-43. https://doi.org/10.1080/09602010802091183
Donaghy ME. Exercise can seriously improve your mental health: Fact or fiction? Adv Physiother. 2007;9:76-88. https://doi.org/10.1080/14038190701395838
van den Kommer TN, Dik MG, Comijs HC, Jonker C, Deeg DJ. Role of lipoproteins and inflammation in cognitive decline: Do they interact? Neurobiol Aging. 2012;33:196.e1-12. https://doi.org/10.1016/j.neurobiolaging.2010.05.024
Varady KA, Bhutani S, Klempel MC, Kroeger CM. Comparison of effects of diet versus exercise weight loss regimens on LDL and HDL particle size in obese adults. Lipids Health Dis. 2011;10:119-23. https://doi.org/10.1186/1476-511X-10-119
Kelley GA, Kelley KS, Roberts S, Haskell W. Combined effects of aerobic exercise and diet on lipids and lipoproteins in overweight and obese adults: A meta-analysis. J Obes. 2012;2012:985902. https://doi.org/10.1155/2012/985902
Crisby M, Bronge L, Wahlund LO. Low levels of high density lipoprotein increase the severity of cerebral white matter changes: Implications for prevention and treatment of cerebrovascular diseases. Curr Alzheimer Res. 2010;7:534-39. https://doi.org/10.2174/156720510792231694
Lehto SM, Niskanen L, Tolmunen T, Hintikka J, Viinamäki H, Heiskanen T, et al. Low serum HDL-cholesterol levels are associated with long symptom duration in patients with major depressive disorder. Psychiatry Clin Neurosci. 2010;64:279-83. https://doi.org/10.1111/j.1440-1819.2010.02079.x
Toyama K, Sugiyama S, Oka H, Hamada M, Iwasaki Y, Horio E, et al. A pilot study: The beneficial effects of combined statin-exercise therapy on cognitive function in patients with coronary artery disease and mild cognitive decline. Intern Med. 2017;56:641-9. https://doi.org/10.2169/internalmedicine.56.7703
Beaman SRd, Beaman PE, García-Peña C, Villa MA, Heres J, Córdova A, et al. Validation of a modified version of the Mini-Mental State Examination (MMSE) in Spanish. Neuropsychol Dev Cogn B Aging Neuropsychol Cogn. 2004;11:1-11.
Folstein MF, Folstein SE, McHugh PR. “Mini-mental state”. A practical method for grading the cognitive state of patients for the clinician. J Psychiatr Res. 1975;12:189-98. https://doi.org/10.1016/0022-3956(75)90026-6
Lourenço RA, Veras RP. Mini-mental state examination: Psychometric characteristics in elderly outpatients. Rev Saúde Pública. 2006;40:712-9. https://doi.org/10.1590/S0034-89102006000500023
Mossberg KA, Fortini E. Responsiveness and validity of the six-minute walk test in individuals with traumatic brain injury. Phys Ther. 2012;92:726-33. https://doi.org/10.2522/ptj.20110157
Larsson UE, Reynisdottir S. The six-minute walk test in outpatients with obesity: Reproducibility and known group validity. Physiother Res Int. 2008;13:84-93. https://doi.org/10.1002/pri.398
Pollentier B, Irons SL, Benedetto CM, DiBenedetto A, Loton D, Seyler RD, et al. Examination of the six minute walk test to determine functional capacity in people with chronic heart failure: A systematic review. Cardiopulm Phys Ther J. 2010;21:13-21.
Fowler RM, Jenkins SC, Maiorana AJ, Gain KR, O’Driscoll G, Gabbay E. Measurement properties of the 6-min walk test in individuals with exercise-induced pulmonary arterial hypertension. Intern Med J. 2011;41:679-87. https://doi.org/10.1111/j.1445-5994.2011.02501.x
Laskin JJ, Bundy S, Moore H, Swanson M, Thies H, Blair M. Using a treadmill for the six minute walk test: Reliability and validity. J Cardiopulm Rehabil Prev. 2007;27:407-10. https://doi.org/10.1097/01.HCR.0000300270.45881.d0
Tveter AT, Dagfinrud H, Moseng T, Holm I. Measuring health-related physical fitness in physiotherapy practice: Reliability, validity, and feasibility of clinical field tests and a patient-reported measure. J Orthop Sports Phys Ther. 2014;44:206-16. https://doi.org/10.2519/jospt.2014.5042
Cohen J. Statistical Power Analysis for the Behavioral Sciences. Second edition. Hillsdale, NJ: L. Erlbaum Associates; 1988. p. 20-27
World Medical Association. Declaration of Helsinki - Ethical principles for medical research involving human subjects. World Med J. 2013;59:199-202.
Sparks DL, Kryscio RJ, Connor DJ, Sabbagh MN, Sparks LM, Lin Y, et al. Cholesterol and cognitive performance in normal controls and the influence of elective statin use after conversion to mild cognitive impairment: Results in a clinical trial cohort. Neurodegener Dis. 2010;7:183-6. https://doi.org/10.1159/000295660
Petersen RC. Mild cognitive impairment as a diagnostic entity. J Intern Med. 2004;256:183-94. https://doi.org/10.1111/j.1365-2796.2004.01388.x
Winblad B, Palmer K, Kivipelto M, Jelic V, Fratiglioni L, Wahlund LO, et al. Mild cognitive impairment - Beyond controversies, towards a consensus: Report of the International Working Group on Mild Cognitive Impairment. J Intern Med. 2004;256:240-6. https://doi.org/10.1111/j.1365-2796.2004.01380.x
Bernick C, Katz R, Smith NL, Rapp S, Bhadelia R, Carlson M, et al. Statins and cognitive function in the elderly: The Cardiovascular Health Study. Neurology. 2005;65:1388-94. https://doi.org/10.1212/01.wnl.0000182897.18229.ec
Rojas-Fernández CH, Cameron J-CF. Is statin-associated cognitive impairment clinically relevant? A narrative review and clinical recommendations. Ann Pharmacother. 2012;46:549-57. https://doi.org/10.1345/aph.1Q620
Ihara M, Okamoto Y, Hase Y, Takahashi R. Association of physical activity with the visuospatial/executive functions of the montreal cognitive assessment in patients with vascular cognitive impairment. J Stroke Cerebrovasc Dis. 2013;22:e146-e51. https://doi.org/10.1016/j.jstrokecerebrovasdis.2012.10.007
Barnes DE, Yaffe K, Satariano WA, Tager IB. A longitudinal study of cardiorespiratory fitness and cognitive function in healthy older adults. J Am Geriatr Soc. 2003;51:459-65. https://doi.org/10.1046/j.1532-5415.2003.51153.x
Cherry BJ, Zettel-Watson L, Chang JC, Shimizu R, Rutledge DN, Jones CJ. Positive associations between physical and cognitive performance measures in fibromyalgia. Arch Phys Med Rehabil. 2012;93:62-71. https://doi.org/10.1016/j.apmr.2011.08.006
Wilbur J, Márquez DX, Fogg L, Wilson RS, Staffileno BA, Hoyem RL, et al. The relationship between physical activity and cognition in older latinos. J Gerontol B Psychol Sci Soc Sci. 2012;67:525-34. https://doi.org/10.1093/geronb/gbr137
Kelly RB. Diet and exercise in the management of hyperlipidemia. Am Fam Physician. 2010;81:1097-102.
Jafri H, Alsheikh-Ali AA, Karas RH. Meta-analysis: Statin therapy does not alter the association between low levels of high-density lipoprotein cholesterol and increased cardiovascular risk. Ann Intern Med. 2010;153:800-8. https://doi.org/10.7326/0003-4819-153-12-201012210-00006
Tziomalos K, Athyros VG, Karagiannis A, Mikhailidis DP. Dyslipidemia as a risk factor for ischemic stroke. Curr Top Med Chem. 2009;9:1291-7. https://doi.org/10.2174/156802609789869628
Kelley GA, Kelley KS. Aerobic exercise and HDL2-C: A meta-analysis of randomized controlled trials. Atherosclerosis. 2006;184:207-15. https://doi.org/10.1016/j.atherosclerosis.2005.04.005
Mikus CR, Boyle LJ, Borengasser SJ, Oberlin DJ, Naples SP, Fletcher J, et al. Simvastatin impairs exercise training adaptations. J Am Coll Cardiol. 2013;62:709-14. https://doi.org/10.1016/j.jacc.2013.02.074
Feuerstein JS, Bjerke WS. Powdered red yeast rice and plant stanols and sterols to lower cholesterol. J Diet Suppl. 2012;9:110-5. https://doi.org/10.3109/19390211.2012.682645
Toyama K, Sugiyama S, Oka H, Iwasaki Y, Sumida H, Tanaka T, et al. Combination treatment of rosuvastatin or atorvastatin, with regular exercise improves arterial wall stiffness in patients with coronary artery disease. PLoS One. 2012;7:e41369. https://doi.org/10.1371/journal.pone.0041369
Weng TC, Yang YHK, Lin SJ, Tai SH. A systematic review and meta-analysis on the therapeutic equivalence of statins. J Clin Pharm Ther. 2010;35:139-51. https://doi.org/10.1111/j.1365-2710.2009.01085.x
Hagner W, Hagner-Derengowska M, Wiacek M, Zubrzycki IZ. Changes in level of VO2max, blood lipids, and waist circumference in the response to moderate endurance training as a function of ovarian aging. Menopause. 2009;16:1009-13. https://doi.org/10.1097/gme.0b013e31819c0924
Weinstein A, Erickson K. Healthy body equals healthy mind. Generations. 2011;35:92-8.
| Estadísticas de artículo | |
|---|---|
| Vistas de resúmenes | |
| Vistas de PDF | |
| Descargas de PDF | |
| Vistas de HTML | |
| Otras vistas | |

























