Mucormycosis: A sweet enemy, case series
Abstract
Mucormycosis is a rare fungal infection caused by fungi of the Mucorales order that occurs in immunocompromised individuals or with loss of skin or mucosa barrier integrity.
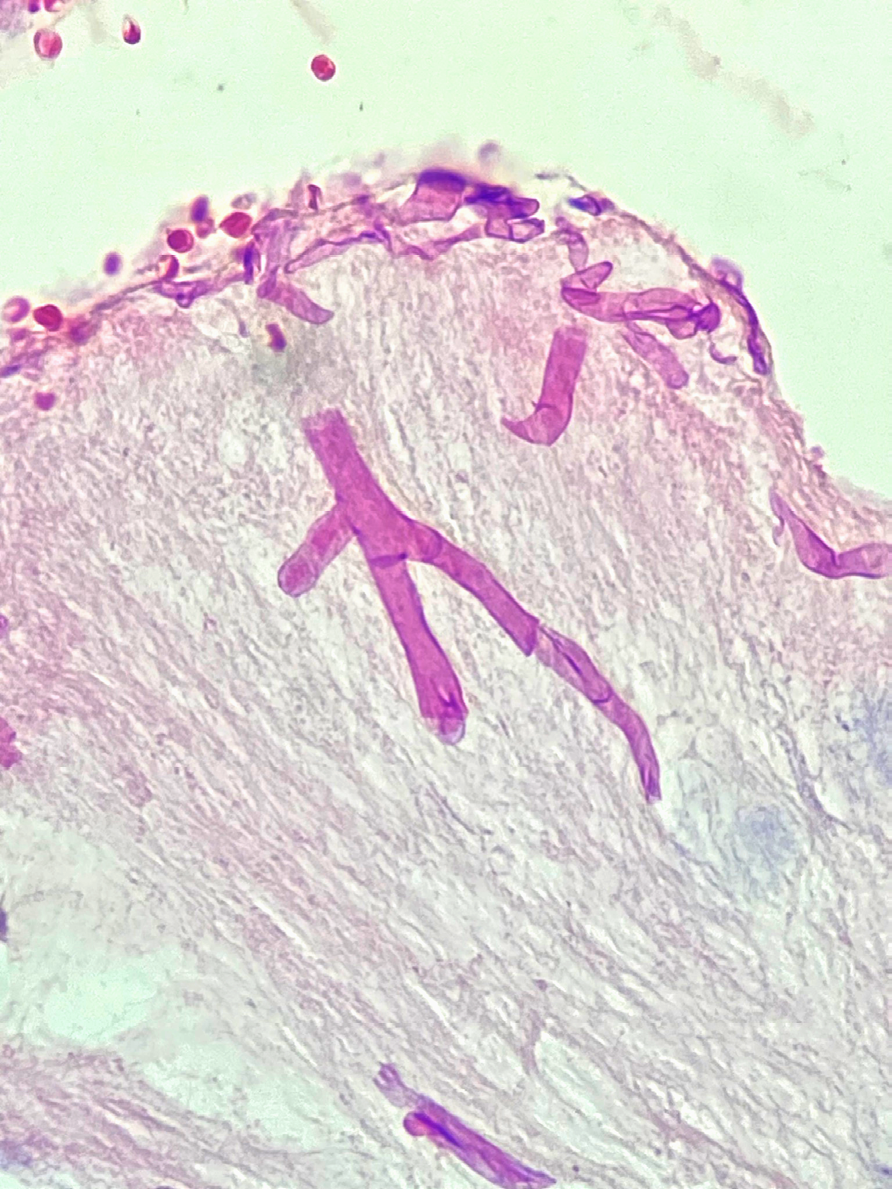
This report presents four cases of rhinocerebral mucormycosis attended at a third-level hospital in Cali (Colombia) during a period of three years. All patients had different case histories and times of evolution. All four had a previous or de novo diagnosis of type 2 diabetes mellitus, with glycated hemoglobin higher than 10% on admission. We ruled out other possible pathologies that could explain their immunocompromised condition. Mucormycosis diagnosis was made with direct visualization of hyaline coenocytic hyphae on biopsies.
The basis of treatment was liposomal amphotericin B and surgical debridement. Two patients presented bacterial coinfection. One asked for voluntary discharge without having completed the treatment, and another one died. The remaining two have attended controls and had an adequate evolution.
Downloads
References
Acosta-España JD, Voigt K. Mini review: Risk assessment, clinical manifestation, prediction, and prognosis of mucormycosis: Implications for pathogen- and human-derived biomarkers. Front Microbiol. 2022;13:895989. https://doi.org/10.3389/fmicb.2022.895989
Bennett JE, Dolin R, Blaser MJ. Mandell, Douglas, and Bennett. Principles and Practice of Infectious Diseases. España: Elsevier; 2019. p. 3117-30. https://doi.org/10.1016/C2012-1-00075-6
Cornely OA, Alastruey-Izquierdo A, Arenz D, Chen SCA, Dannaoui E, Hochhegger B, et al. Global guideline for the diagnosis and management of mucormycosis: An initiative of the European Confederation of Medical Mycology in cooperation with the Mycoses Study Group Education and Research Consortium. Lancet Infect Dis. 2019;19:e405-e21. https://doi.org/10.1016/S1473-3099(19)30312-3
Nucci M, Engelhardt M, Hamed K. Mucormycosis in South America: A review of 143 reported cases. Mycoses. 2019;62:730-8. https://doi.org/10.1111/myc.12958
Prakash H, Chakrabarti A. Global epidemiology of mucormycosis. J Fungi (Basel). 2019;5. https://doi.org/10.3390/jof5010026
Bravo JH, Agudelo AM, Cortés A, Matta L. Mucormicosis rino-órbito-cerebral de origen dental. Biomédica. 2018;38:27-31. https://doi.org/10.7705/biomedica.v38i0.3383
Rammaert B, Lanternier F, Poirée S, Kania R, Lortholary O. Diabetes and mucormycosis: A complex interplay. Diabetes Metab. 2012;38:193-204. https://doi.org/10.1016/j.diabet.2012.01.002
Binder U, Maurer E, Lass-Flörl C. Mucormycosis – from the pathogens to the disease. Clin Microbiol Infect. 2014;20:60-6. https://doi.org/10.1111/1469-0691.12566
Gamaletsou MN, Sipsas NV, Roilides E, Walsh TJ. Rhino-orbital-cerebral mucormycosis. Curr Infect Dis Rep. 2012;14:423-34. https://doi.org/10.1007/s11908-012-0272-6
Berbudi A, Rahmadika N, Tjahjadi AI, Ruslami R. Type 2 diabetes and its impact on the immune system. Curr Diabetes Rev. 2020;16:442-9. https://doi.org/10.2174/1573399815666191024085838
Ibrahim AS, Spellberg B, Walsh TJ, Kontoyiannis DP. Pathogenesis of mucormycosis. Clin Infect Dis. 2012;54(Suppl.1):S16-22 2012;54(Suppl.1):S16-22. https://doi.org/10.1093/cid/cir865
Farmakiotis D, Kontoyiannis DP. Mucormycoses. Infect Dis Clin North Am. 2016;30:143-63. https://doi.org/10.1016/j.idc.2015.10.011
Sun HY, Forrest G, Gupta KL, Aguado JM, Lortholary O, Julia MB, et al. Rhino-orbitalcerebral zygomycosis in solid organ transplant recipients. Transplantation. 2010;90:85-92. https://doi.org/10.1097/tp.0b013e3181dde8fc
Chamilos G, Lewis RE, Kontoyiannis DP. Delaying amphotericin B-based frontline therapy significantly increases mortality among patients with hematologic malignancy who have zygomycosis. Clin Infect Dis. 2008;47:503-9. https://doi.org/10.1086/590004
Ibrahim AS, Bowman JC, Avanessian V, Brown K, Spellberg B, Edwards JE, Jr., et al. Caspofungin inhibits Rhizopus oryzae 1,3-beta-D-glucan synthase, lowers burden in brain measured by quantitative PCR, and improves survival at a low but not a high dose during murine disseminated zygomycosis. Antimicrob Agents Chemother. 2005;49:721-7. https://doi.org/10.1128/AAC.49.2.721-727.2005
Ferguson BJ, Mitchell TG, Moon R, Camporesi EM, Farmer J. Adjunctive hyperbaric oxygen for treatment of rhinocerebral mucormycosis. Rev Infect Dis. 1988;10:551-9. https://doi.org/10.1093/clinids/10.3.551
Copyright (c) 2024 Biomedica

This work is licensed under a Creative Commons Attribution 4.0 International License.
| Article metrics | |
|---|---|
| Abstract views | |
| Galley vies | |
| PDF Views | |
| HTML views | |
| Other views | |

























