Effectiveness of interventions for the reversal of a metabolic syndrome diagnosis: An update of a meta-analysis of mixed treatment comparison studies
Abstract
Introduction: Identifying the most effective interventions to reverse the metabolic syndrome can be key in the design of clinical strategies to prevent progression to type 2 diabetes mellitus and cardiovascular disease.
Objective: To estimate the effect size of the interventions used for the reversal of metabolic syndrome.
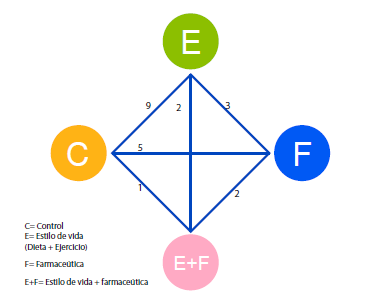
Materials and methods: We searched in Embase and Medline databases for randomized clinical trials with an outcome defined as the reversal of the metabolic syndrome diagnosis. We classified the interventions in four dimensions: 1) lifestyle (diet and exercise); 2) pharmaceuticals; 3) a combination of both, and 4) control groups, and we conducted a mixed treatment comparison analysis.
Results: Additional to the previous meta-analysis published by Dunkley, et al. in 2012, we dentified two other studies. Lifestyle interventions had 2.61 more chances to achieve the reversal of the metabolic syndrome than the control group, with a credible interval between 1.00 and 5.47. Pharmaceutical treatments showed a 3.39 higher chance of reversing the syndrome compared with the control group, but the credible interval was estimated from 0.81 to 9.99. Lifestyle interventions had 1.59 more chance of reversal than the pharmaceutical treatments.
Conclusion: Diet and physical activity-based interventions had a higher probability of effectiveness to reverse a metabolic syndrome diagnosis.
Downloads
References
O’neill S, O’driscoll L. Metabolic syndrome: A closer look at the growing epidemic and its associated pathologies. Obes Rev. 2015;16:1-12. https://doi.org/10.1111/obr.12229
Balkau B, Charles MA, Drivsholm T, Borch-Johnsen K, Wareham N, Yudkin JS, et al. Frequency of the WHO metabolic syndrome in European cohorts, and an alternative definition of an insulin resistance syndrome. Diabet Metab. 2002;28:364-76.
Cameron AJ, Shaw JE, Zimmet PZ. The metabolic syndrome: Prevalence in worldwide populations. Endocrinol Metab Clin North Am. 2004;33:351-75. https://doi.org/10.1016/j.ecl.2004.03.005
Aguilar-Salinas CA, Rojas R, Gómez-Pérez FJ, Valles V, Ríos-Torres JM, Franco A, et al. Analysis of the agreement between the World Health Organization criteria and the National Cholesterol Education Program-III definition of the metabolic syndrome: Results from a population-based survey. Diabetes Care. 2003;26:1635. https://doi.org/10.2337/diacare.26.5.1635
Villegas R, Perry IJ, Creagh D, Hinchion R, O’Halloran D. Prevalence of the metabolic syndrome in middle-aged men and women. Diabetes Care. 2003;26:3198-9. https://doi.org/10.2337/diacare.26.11.3198-a
Ford ES, Giles WH, Dietz WH. Prevalence of the metabolic syndrome among US adults: Findings from the Third National Health and Nutrition Examination Survey. JAMA. 2002;287:356-9. https://doi:10.1001/jama.287.3.356
Gupta A, Gupta R, Sarna M, Rastogi S, Gupta VP, Kothari K. Prevalence of diabetes, impaired fasting glucose and insulin resistance syndrome in an urban Indian population. Diab Res Clin Pract. 2003;61:69-76. https://doi.org/10.1016/S0168-8227(03)00085-8
Zimmet P, Shaw J, Alberti KG. Preventing type 2 diabetes and the dysmetabolic syndrome in the real world: A realistic view. Diabet Med. 2003;20:693-702. https://doi.org/10.1046/j.1464-5491.2003.01052.x
Gami AS, Witt BJ, Howard DE, Erwin PJ, Gami LA, Somers VK, et al. Metabolic syndrome and risk of incident cardiovascular events and death: A systematic review and meta-analysis of longitudinal studies. J Am Coll Cardiol. 2007;49:403-14. https://doi.org/10.1016/j.jacc.2006.09.032
Mottillo S, Filion KB, Genest J, Joseph L, Pilote L, Poirier P, et al. The metabolic syndrome and cardiovascular risk: A systematic review and meta-analysis. J Am Coll Cardiol. 2010;56:1113-32. https://doi.org/10.1016/j.jacc.2010.05.034
Ford ES, Li C, Sattar N. Metabolic syndrome and incident diabetes: Current state of the evidence. Diabetes Care. 2008;31:1898-904. https://doi.org/10.2337/dc08-0423
Dunkley AJ, Charles K, Gray LJ, Camosso-Stefinovic J, Davies MJ, Khunti K. Effectiveness of interventions for reducing diabetes and cardiovascular disease risk in people with metabolic syndrome: Systematic review and mixed treament comparison meta-analysis. Diabetes Obes Metab. 2012;14:616-25. https://doi.org/10.1111/j.1463-1326.2012.01571.x
García-Perdomo HA, Tobías A. Metanálisis en red: comparaciones indirectas y mixtas, un nuevo método al servicio de la epidemiología clínica y la salud pública. Rev Perú Med Exp Salud Pública. 2016;33:149-53. https://doi.org/10.17843/rpmesp.2016.331.1889
Higgins J, Green S. Cochrane Handbook for Systematic Reviews of Interventions, Version 5.1.0. The Cochrane Collaboration; 2011. Disponible en: https://handbook-5-1.cochrane.org/
Bucher H, Guyatt GH, Griffith L, Walter SD. The results of direct and indirect treatment comparisons in meta-analysis of randomized controlled trials. J Clin Epidemiol. 1997;50:683-91. https://doi.org/10.1016/S0895-4356(97)00049-8
Coleman CI, Phung OJ, Cappelleri JC, Baker WL, Kluger J, White CM, et al. Use of mixed treatment comparisons in systematic reviews. 2012. Rockville, MD: Agency for Healthcare Research and Quality; 2012.
Salanti G, Higgins JP, Ades AE, Ioannidis JP. Evaluation of networks of randomized trials. Stat Methods Med Res. 2008;17:279-301. https://doi.org/10.1177/0962280207080643
Gutiérrez-Pulido H, Gutiérrez-González P. Fundamentos y aplicaciones de la estadística Bayesiana. México: Universidad de Guadalajara; 2013.
Sutton AJ, Abrams KR. Bayesian methods in meta-analysis and evidence synthesis. Stat Methods Med Res. 2001;10:277-303. https://doi.org/10.1177/096228020101000404
Song F, Altman DG, Glenny AM, Deeks JJ. Validity of indirect comparison for estimating efficacy of competing interventions: Empirical evidence from published meta-analyses. BMJ. 2003;326:472. https://doi.org/10.1136/bmj.326.7387.472
Lam SK, Owen A. Combined resynchronisation and implantable defibrillator therapy in left ventricular dysfunction: Bayesian network meta-analysis of randomised controlled trials. BMJ. 2007;335:925. https://doi.org/10.1136/bmj.39343.511389.BE
Cooper NJ, Sutton AJ, Morris D, Ades AE, Welton NJ. Addressing between-study heterogeneity and inconsistency in mixed treatment comparisons: Application to stroke prevention treatments in individuals with non-rheumatic atrial fibrillation. Stat Med. 2009;28:1861-81. https://doi.org/10.1002/sim.3594
Moher D, Liberati A, Tetzlaff J, Altman DG. Preferred reporting items for systematic reviews and meta-analyses: The PRISMA statement. Ann Intern Med. 2009;151:264-9. https://doi.org/10.7326/0003-4819-151-4-200908180-00135
Yoo S, Kim H, Cho HI. Improvements in the metabolic syndrome and stages of change for lifestyle behaviors in Korean older adults. Osong Public Health Res Pespect. 2012;3:85-93. https://doi.org/10.1016/j.phrp.2012.04.007
Siu PM, Angus PY, Benzie IF, Woo J. Effects of 1-year yoga on cardiovascular risk factors in middle-aged and older adults with metabolic syndrome: A randomized trial. Diabetol Metab Syndr. 2015;7:40. https://doi.org/10.1186/s13098-015-0034-3
Anderssen S, Carroll S, Urdal P, Holme I. Combined diet and exercise intervention reverses the metabolic syndrome in middle-aged males: Results from the Oslo Diet and Exercise Study. Scand J Med Sci Sports. 2007;17:687. https://doi.org/10.1111/j.1600-0838.2006.00631.x
Athyros VG, Mikhailidis DP, Papageorgiou AA, Didangelos TP, Peletidou A, Kleta D, et al. Targeting vascular risk in patients with metabolic syndrome but without diabetes. Metabolism. 2005;54:1065-74. https://doi.org/10.1016/j.metabol.2005.03.010
Bo S, Ciccone G, Baldi C, Benini L, Dusio F, Forastiere G, et al. Effectiveness of a lifestyle intervention on metabolic syndrome. A randomized controlled trial. J Gen Intern Med. 2007;22:1695-703. https://doi.org/10.1007/s11606-007-0399-6
Esposito K, Marfella R, Ciotola M, Di Palo C, Giugliano F, Giugliano G, et al. Effect of a mediterranean-style diet on endothelial dysfunction and markers of vascular inflammation in the metabolic syndrome a randomized trial. JAMA. 2004;292:1440-6. https://doi.org/10.1001/jama.292.12.1440
Esposito K, Ciotola M, Carleo D, Schisano B, Saccomanno F, Sasso FC, et al. Effect of rosiglitazone on endothelial function and inflammatory markers in patients with the metabolic syndrome. Diabetes Care. 2006;29:1071-6. https://doi.org/10.2337/dc05-2174
Geluk CA, Asselbergs FW, Hillege HL, Bakker SJ, de Jong PE, Zijlstra F. Impact of statins in microalbuminuric subjects with the metabolic syndrome: A substudy of the PREVEND intervention trial. Eur Heart J. 2005;26:1314-20. https://doi.org/10.1093/eurheartj/ehi253
Johnson JL, Slentz CA, Houmard JA, Samsa GP, Duscha BD, Aiken LB, et al. Exercise training amount and intensity effects on metabolic syndrome (from studies of a targeted risk reduction intervention through defined exercise). Am J Cardiol. 2007;100:1759-66. https://doi.org/10.1016/j.amjcard.2007.07.027
Orchard TJ, Temprosa M, Goldberg R, Haffner S, Ratner R, Marcovina S, et al. The effect of metformin and intensive lifestyle intervention on the metabolic syndrome: The Diabetes Prevention Program randomized trial. Ann Intern Med. 2005;142:611-9. https://doi.org/10.7326/0003-4819-142-8-200504190-00009
Phelan S, Wadden TA, Berkowitz RI, Sarwer DB, Womble LG, Cato RK, et al. Impact of weight loss on the metabolic syndrome. Int J Obes. 2007;31:1442-8. https://doi.org/10.1038/sj.ijo.0803606
Ramachandran A, Snehalatha C, Satyavani K, Sivasankari S, Vijay V. Metabolic syndrome does not increase the risk of conversion of impaired glucose tolerance to diabetes in Asian Indians: Result of Indian diabetes prevention programme. Diabetes Res Clin Pract. 2007;76:215-8. https://doi.org/10.1016/j.diabres.2006.08.009
Stewart KJ, Bacher AC, Turner K, Lim JG, Hees PS, Shapiro EP, et al. Exercise and risk factors associated with metabolic syndrome in older adults. Am J Prev Med. 2005;28:9-18. https://doi.org/10.1016/j.amepre.2004.09.006
van Gaal LF, Rissanen AM, Scheen AJ, Ziegler O, Rössner S; RIO-Europe Study Group. Effects of the cannabinoid-1 receptor blocker rimonabant on weight reduction and
cardiovascular risk factors in overweight patients: 1-year experience from the RIO-Europe study. Lancet. 2005;365:1389-97. https://doi.org/10.1016/S0140-6736(05)66374-X
Villareal DT, Miller BV, Banks M, Fontana L, Sinacore DR, Klein S. Effect of lifestyle intervention on metabolic coronary heart disease risk factors in obese older adults. Am J Clin Nutr. 2006;84:1317-23. https://doi.org/10.1093/ajcn/84.6.1317
Some similar items:
- Álvaro Javier Idrovo, Luz Helena Sanín, Adverse reproductive outcomes among women working in Colombian floriculture: a summary of the evidence through metaanalysis , Biomedica: Vol. 27 No. 4 (2007)
- Alicia Norma Alayón, Saudith Ariza, Karen Baena, Lina Lambis, Lina Martínez, Lourdes Benítez, Active search and assessment of cardiovascular risk factors in young adults, Cartagena de Indias, 2007 , Biomedica: Vol. 30 No. 2 (2010)
- Sandra Moreno, Beatriz Parra, Javier E. Botero, Freddy Moreno, Daniel Vásquez, Hugo Fernández, Sandra Alba, Sara Gallego, Gilberto Castillo, Adolfo Contreras, Periodontal microbiota and microorganisms isolated from heart valves in patients undergoing valve replacement surgery in a clinic in Cali, Colombia , Biomedica: Vol. 37 No. 4 (2017)
- Norma Cecilia Serrano-Díaz, Edna Magaly Gamboa-Delgado, Clara Lucía Domínguez-Urrego, Andrea Liliana Vesga-Varela, Sergio Eduardo Serrano-Gómez, Doris Cristina Quintero-Lesmes, Vitamin D and risk of preeclampsia: A systematic review and meta-analysis , Biomedica: Vol. 38 No. Sup.1 (2018): Suplemento 1, Enfermedades crónicas
- Nora Alejandra Zuluaga, Adriana Osorno, Alba Lozano, Oscar Villada, Clinical and metabolic effect of a multidisciplinary intervention through a comprehensive care program for children and adolescents with obesity , Biomedica: Vol. 40 No. 1 (2020)
| Article metrics | |
|---|---|
| Abstract views | |
| Galley vies | |
| PDF Views | |
| HTML views | |
| Other views | |

























