Profile of antiretroviral agents use in Colombia
Abstract
Introduction: Since the beginning of the epidemic, human immunodeficiency virus (HIV) has taken more than 36 million lives.
Objective: To determine the antiretroviral drug prescription patterns in a population of individuals with HIV infection in Colombia.
Materials and methods: Cross-sectional study analyzing the profiles of patients treated with antiretroviral drugs between April 1st and September 30th, 2015. The sociodemographic, pharmacological, and comorbidity variables were identified. Individuals with a positive diagnosis of HIV of all ages and both genders were included.
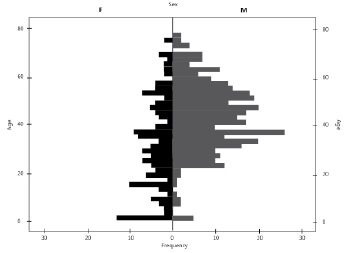
Results: We found 641 patients with a mean age of 39.0±17 years who were predominantly male (60.2%). The most used medications were lamivudine-zidovudine (51.6%), lopinavir-ritonavir (36%) and efavirenz (24.5%). The combination of lamivudine-zidovudine plus lopinavir-ritonavir was the most prescribed regimen (29.5%), but a total of 80 different regimens was identified. Being an adult between the ages of 45-64 years (OR=2.25; 95%CI 1.367-3.713) was associated with a greater probability
of receiving 4 or more antiretrovirals. A total of 267 (41.6%) patients used at least one comedication (range: 1-18 drugs), especially anti-ulcer (57.3%), lipid-lowering (28.8%) and anti-hypertensive (28.5%) drugs.
Conclusions: Patients undergoing antiretroviral treatment are receiving medications with elevated intrinsic values at the recommended doses and present comorbidities associated with chronic agerelated conditions. However, these patients receive a great variety of regimens that are not included in the clinical practice guidelines.
Downloads
References
Kharsany AB, Karim QA. HIV Infection and AIDS in Sub-Saharan Africa: Current status, challenges and opportunities. Open AIDS J. 2016;10:34-48. https://doi.org/10.2174/1874613601610010034
Friedland G. Marking time in the Global HIV/AIDS pandemic. JAMA. 2016;316:145-6. https://doi.org/10.1001/jama.2016.9006
Fettig J, Swaminathan M, Murrill CS, Kaplan JE. Global epidemiology of HIV. Infect Dis Clin North Am. 2014;28:323-37. https://doi.org/10.1016/j.idc.2014.05.001
Sabin CA, Lundgren JD. The natural history of HIV infection. Curr Opin HIV AIDS. 2013;8:311-7. https://doi. org/10.1097/COH.0b013e328361fa66
Hammer SM. Clinical practice. Management of newly diagnosed HIV infection. N Engl J Med. 2005;353:1702-10. https://doi.org/10.1056/NEJMcp051203
Esté JA, Cihlar T. Current status and challenges of antiretroviral research and therapy. Antiviral Res. 2010;85:25-33. https://doi.org/10.1016/j.antiviral.2009.10.007
Pau AK, George JM. Antiretroviral therapy: Current drugs. Infect Dis Clin North Am. 2014;28:371-402. https://doi.org/10.1016/j.idc.2014.06.001
Sawyer JR, Ma Q, Hsiao CB. Single-tablet, once-daily treatment regimens for HIV. Lancet Infect Dis. 2014;14:265-7. https://doi.org/10.1016/S1473-3099(14)70026-X
Volberding PA, Deeks SG. Antiretroviral therapy and management of HIV infection. Lancet. 2010;376:49-62. https://doi.org/10.1016/S0140-6736(10)60676-9
Maartens G, Celum C, Lewin SR. HIV infection: Epidemiology, pathogenesis, treatment, and prevention. Lancet. 2014;384:258-71. https://doi.org/10.1016/S0140-6736(14)60164-1
Machado JE, Alzate JA. Patrones de prescripción de antirretrovirales en 997 pacientes colombianos. Biomédica. 2008;28:78-86. https://doi.org/10.7705/biomedica. v28i1.110
Machado-Alba JE, Vidal X. Effectiveness of antiretroviral treatment in Colombia. Rev Panam Salud Pública. 2012;32:360-7.
Günthard HF, Aberg JA, Eron JJ, Hoy JF, Telenti A, Benson CA, et al. International Antiviral Society-USA Panel. Antiretroviral treatment of adult HIV infection: 2014 recommendations of the International Antiviral Society-USA Panel. JAMA. 2014;312:410-25. https://doi.org/10.1001/jama.2014.8722
Johnson JA, Sax PE. Beginning antiretroviral therapy for patients with HIV. Infect Dis Clin North Am. 2014;28:421-38. https://doi.org/10.1016/j.idc.2014.06.003
Crawford KW, Ripin DH, Levin AD, Campbell JR, Flexner C, participants of Conference on Antiretroviral Drug Optimization. Optimising the manufacture, formulation, and dose of antiretroviral drugs for more cost-efficient delivery in resource-limited settings: A consensus statement. Lancet Infect Dis. 2012;12:550-60. https://doi.org/10.1016/S1473-3099(12)70134-2
Werneck-Silva AL, Prado IB. Dyspepsia in HIV-infected patients under highly active antiretroviral therapy. J Gastroenterol Hepatol. 2007;22:1712-6. https://doi.org/10. 1111/j.1440-1746.2007.04897.x
Dagenais-Lussier X, Mouna A, Routy JP, Tremblay C, Sekaly RP, El-Far M, et al. Current topics in HIV-1 pathogenesis: The emergence of deregulated immunometabolism
in HIV-infected subjects. Cytokine Growth Factor Rev. 2015;26:603-13. https://doi.org/10.1016/j.cytogfr.2015.09.001
Amariles P, Giraldo NA, Faus MJ. Interacciones medicamentosas en pacientes infectados con el VIH: aproximación para establecer y evaluar su relevancia clínica. Farm Hosp. 2007;31:283-302.
Silverberg MJ, Leyden W, Horberg MA, DeLorenze GN, Klein D, Quesenberry CP. Older age and the response to and tolerability of antiretroviral therapy. Arch Intern Med. 2007;167:684-91. https://doi.org/10.1001/archinte.167.7.684
Martin CP, Fain MJ, Klotz SA. The older HIV-positive adult: A critical review of the medical literature. Am J Med. 2008;121:1032-7. https://doi.org/10.1016/j.amjmed.2008.08.009
Luther VP, Wilkin AM. HIV infection in older adults. Clin Geriatr Med. 2007;23:567-83. https://doi.org/10.1016/j.cger.2007.02.004
Cardoso SW, Torres TS, Santini-Oliveira M, Marins LMS, Veloso VG, Grinsztejn B. Aging with HIV: A practical review. Braz J Infect Dis. 2013;17:464-79. https://doi.org/10.1016/j.bjid.2012.11.007
Cottrell ML, Hadzic T, Kashuba AD. Clinical pharmacokinetic, pharmacodynamics and drug-interaction profile of the integrase inhibitor dolutegravir. Clin Pharmacokinet. 2013;52:981-94. https://doi.org/10.1007/s40262-013-0093-2
Some similar items:
- María Patricia Arbeláez, Alexánder Arbeláez, Rubén Darío Gómez, Carlos Rojas, Lázaro Vélez, Sonia Luz Arias, Jorge Nagles, Luz Marina Peláez, Gloria Betancourt, Gloria Velásquez, Effectiveness of prophylaxis against tuberculosis in patients infected with HIV , Biomedica: Vol. 27 No. 4 (2007)
- Jorge Machado, John Alexander Alzate, Patterns of antiretroviral drug prescripcion in 997 Colombian patients , Biomedica: Vol. 28 No. 1 (2008)
- Andres Gaviria-Mendoza, Manuel E. Machado-Duque, Jorge E. Machado-Alba, Lipid-lowering drug prescriptions in a group of Colombian patients , Biomedica: Vol. 39 No. 4 (2019)
- Jorge Enrique Machado-Alba, Luis Felipe Calvo-Torres, Andrés Gaviria-Mendoza, Juan Daniel Castrillón-Spitia, Prescribing patterns of antiparkinson drugs in a group of Colombian patients, 2015 , Biomedica: Vol. 38 No. 3 (2018)
- Jorge E. Machado-Alba, Cristhian David Morales-Plaza, Antipsychotic prescription patterns in patients affiliated to the Social Security Health System in Colombia , Biomedica: Vol. 33 No. 3 (2013)
- Alvaro Vallejos, Adverse reactions by antibiotics in a pediatric and neonatal intensive care unit located in Bogotá, Colombia , Biomedica: Vol. 27 No. 1 (2007)
- Rodolfo J. Dennis, Jairo H. Roa, Juan Villadiego, Freddy Méndez, Elías Vieda, Héctor Restrepo, Venous thromboembolism prophylaxis in Colombian surgical and medical patients: Results for Colombia of the ENDORSE study , Biomedica: Vol. 31 No. 2 (2011)
- María Teresa Rugeles, Paula A. Velilla, Carlos J. Montoya, Mechanisms of human natural resistance to HIV: A summary of ten years of research in the Colombian population , Biomedica: Vol. 31 No. 2 (2011)
- Myrtha Arango, Elizabeth Castañeda, Clara Inés Agudelo, Catalina De Bedout, Carlos Andrés Agudelo, Angela Tobón, Melva Linares, Yorlady Valencia, Ángela Restrepo, The Colombian Histoplasmosis Study Group, Histoplasmosis: results of the Colombian National Survey, 1992-2008 , Biomedica: Vol. 31 No. 3 (2011)
- Jorge Andrés Potosí, Yina Marcela Gutiérrez, Fabiola Eugenia González, The relevance of clinical and epidemiological correlation in the early diagnosis of histoplasmosis: report of two clinical cases in Popayán, Colombia , Biomedica: Vol. 43 No. Sp. 1 (2023): Agosto, Micología médica
| Article metrics | |
|---|---|
| Abstract views | |
| Galley vies | |
| PDF Views | |
| HTML views | |
| Other views | |

























