Neuroleptic malignant syndrome associated with acute organophosphate poisoning: Case report
Abstract
Neuroleptic malignant syndrome is a rare and potentially fatal clinical condition frequently associated with the use of antipsychotics. In the literature, there is only one case report associated with the intake of organophosphates.
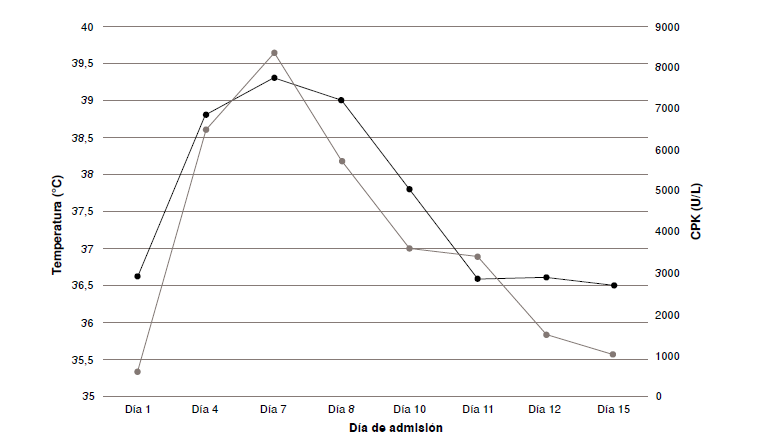
We present the case of a patient who presented with a clinical picture compatible with neuroleptic malignant syndrome, after the ingestion of an organophosphate (chlorpyrifos). A 57-year-old man who consulted for attempted suicide, acute deterioration of consciousness, torpid neurological evolution, and associated autonomic instability associated with rigidity, persistent hyperthermia, and elevated CPK. Bromocriptine treatment was offered, which resolved the clinical picture. The association with the ingestion of an organophosphate was established, and he was discharged without sequelae.
The diagnosis of neuroleptic malignant syndrome is clinical and should be considered in any case of exposure to substances that may lead to dysregulation of dopaminergic neurotransmission in order to initiate timely therapy and impact outcomes.
Downloads
References
Uprety A, Pantha B, Karki L, Nepal SP, Khadka M. Prevalence of intermediate syndrome among admitted patients with organophosphorous poisoning in a tertiary care hospital. JNMA J Nepal Med Assoc. 2019;57:340-3. https://doi.org/10.31729/jnma.4569
Ochi G, Watanabe K, Tokuoka H, Hatakenaka S, Arai T. Neuroleptic malignant-like syndrome: A complication of acute organophosphate poisoning. Can J Anaesth. 1995;42:1027-30. https://doi.org/10.1007/bf03011077
Tse L, Barr AM, Scarapicchia V, Vila-Rodríguez F. Neuroleptic malignant syndrome: A review from a clinically oriented perspective. Curr Neuropharmacol. 2015;13:395-406. https://doi.org/10.2174/1570159x13999150424113345
Modi S, Dharaiya D, Schultz L, Varelas P. Neuroleptic malignant syndrome: Complications, outcomes, and mortality. Neurocrit Care. 2016;24:97-103. https://doi.org/10.1007/s12028-015-0162-5
Singhai K, Kuppili PP, Nebhinani N. Atypical neuroleptic malignant syndrome: A systematic review of case reports. Gen Hosp Psychiatry. 2019;60:12-9. https://doi.org/10.1016/j.genhosppsych.2019.06.009
Torres-Altoro MI, Mathur BN, Drerup JM, Thomas R, Lovinger DM, O’Callaghan JP, et al. Organophosphates dysregulate dopamine signaling, glutamatergic neurotransmission, and induce neuronal injury markers in striatum: Organophosphates dysregulate striatum. J Neurochem. 2011;119:303-13. https://doi.org/10.1111/j.1471-4159.2011.07428.x
Levenson JL. Neuroleptic malignant syndrome. Am J Psychiatry. 1985;142:1137-45. https://doi.org/10.1176/ajp.142.10.1137
Singh N, Lawana V, Luo J, Phong P, Abdalla A, Palanisamy B, et al. Organophosphate pesticide chlorpyrifos impairs STAT1 signaling to induce dopaminergic neurotoxicity: Implications for mitochondria mediated oxidative stress signaling events. Neurobiol Dis. 2018;117:82-113. https://doi.org/10.1016/j.nbd.2018.05.019
Nakamagoe K, Watanabe M, Takeda T, Mizutani T, Tamaoka A. Parkinsonism with organophosphate poisoning. BMJ Case Rep. 2009;2009:bcr0420091766. https://doi.org/10.1136/bcr.04.2009.1766
Hsieh BH, Deng JF, Ger J. La inhibición de la acetilcolinesterasa y el síndrome extrapiramidal: una revisión de la neurotoxicidad de los organofosforados. Neurotoxicology. 2001;22:423-7.
Some similar items:
- Carolina Gómez, Ruth María Eraso, Carlos A. Aguirre, María del Pilar Pérez, Kikuchi-Fujimoto disease: pediatric case presentation , Biomedica: Vol. 30 No. 4 (2010)
- Álvaro A. Faccini-Martínez, Elkin G. Forero-Becerra, Jesús A. Cortés-Vecino, Luis J. Polo-Teran, Jorge H. Jácome, Jimmy J. Vargas, Gustavo Valbuena, Marylin Hidalgo, Probable case of flea-borne spotted fever (Rickettsia felis) , Biomedica: Vol. 33 (2013): Suplemento 1, Fiebres hemorrágicas
- Jefferson Antonio Buendía, Juana Patricia Sánchez-Villamil, Gabriela Urman, Cost-effectiveness of diagnostic strategies of severe bacterial infection in infants with fever without a source , Biomedica: Vol. 36 No. 3 (2016)
- Fernando Rosso, Sara Vanegas, Sarita Rodríguez, Robinson Pacheco, Prevalence and clinical course of dengue infection in elderly patients with acute febrile illness in a tertiary care hospital in Cali, Colombia , Biomedica: Vol. 36 (2016): Suplemento 2, Enfermedades virales
- Eliana Patricia Calvo, Carolina Coronel-Ruiz, Syrley Velazco, Myriam Velandia-Romero, Jaime E. Castellanos, Dengue and Chikungunya differential diagnosis in pediatric patients , Biomedica: Vol. 36 (2016): Suplemento 2, Enfermedades virales
- René Ramírez-García, Juan Carlos Quintero , Aixa Paola Rosado , Margarita Arboleda , Víctor Alejandro González, Piedad Agudelo-Flórez, Leptospirosis and rickettsiosis, a diagnostic challenge for febrile syndrome in endemic areas , Biomedica: Vol. 41 No. 2 (2021)
- Ronald Maestre-Serrano , Zulibeth Flórez-Rivadeneira , Juan Miguel Castro-Camacho, Linda Ochoa-Bohórquez , Doris Gómez-Camargo , Paula Pareja-Loaiza, Gustavo Ponce-García , Adriana E. Flores, Evaluation of susceptibility to organophosphates in populations of Aedes aegypti in La Guajira, Colombia , Biomedica: Vol. 43 No. 2 (2023)
Copyright (c) 2022 Biomedica

This work is licensed under a Creative Commons Attribution 4.0 International License.
| Article metrics | |
|---|---|
| Abstract views | |
| Galley vies | |
| PDF Views | |
| HTML views | |
| Other views | |

























